What the Heck Is a Pessary? Your Guide to Pelvic Organ Prolapse Support
Pelvic organ prolapse, or “POP,” is a common condition often occurring in the postpartum population. POP occurs when the ligaments and/or muscles that support the pelvic organs - bladder, uterus, rectum, vagina - become weak or stretched. As a result, they can bulge into the vaginal canal, causing symptoms that can be uncomfortable or embarrassing.
Treatment options include surgery, physical therapy, or use of a pessary. Pelvic floor physical therapy offers a non-invasive, holistic approach to managing POP symptoms. Keep reading to see how physical therapy can help!
Understanding Pelvic Organ Prolapse
POP is most common in women who have given birth vaginally, gone through menopause, or experienced increased intra-abdominal pressure such as in cases of chronic constipation. The severity can vary, and symptoms can depend on which organ is affected and to what degree it has descended. Common symptoms of pelvic floor dysfunction include:
Feeling of something bulging into the vagina, like a tampon is sticking out (when not wearing a tampon)
Pelvic or perineal heaviness or pressure
Urinary symptoms - increased frequency, leaking, incomplete emptying
Bowel symptoms - incomplete emptying, needing to splint
Low back ache
In more severe cases - bleeding, discharge, infection
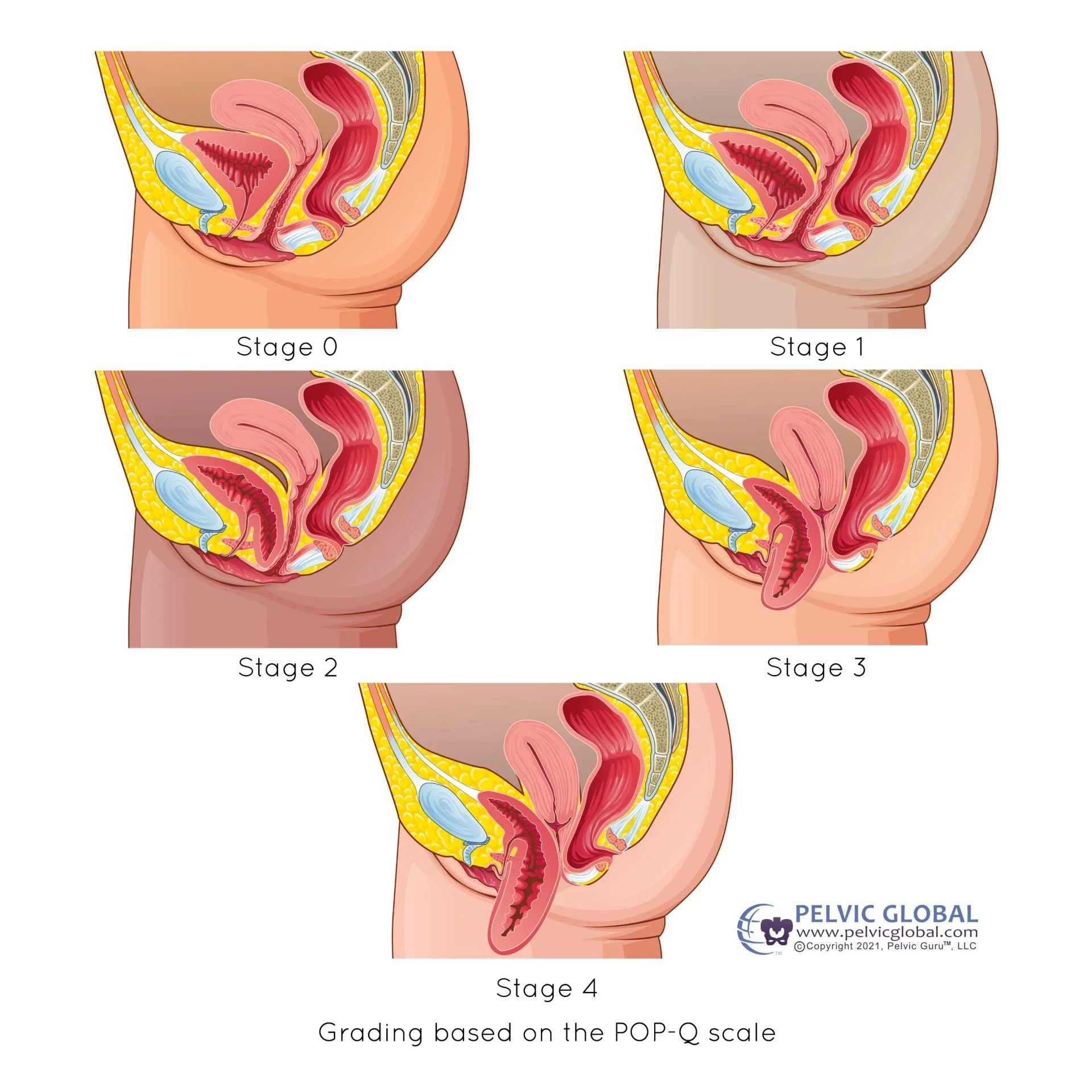
Pelvic organ prolapse is categorized into different stages, with stage 1 being the mildest (where the organs are slightly displaced) and stage 4 being the most severe (where the organs protrude outside the vaginal opening).
The International Urogynaecological Consultation (2021) final consensus defines clinical POP as having descent of at least one vaginal wall to or beyond the hymen, PLUS EITHER: bothersome characteristic symptoms (most commonly vaginal bulge) OR functional or medical compromise due to prolapse.
How can Physical Therapy help in managing POP?
Pelvic floor physical therapy is essential in the management of pelvic organ prolapse. While ligaments suspend the pelvic organs from above, pelvic floor muscles are critical to supporting pelvic organs from the bottom of the abdominal cavity. Maximizing the strength and range of motion of these muscles can help reduce or eliminate symptoms as well as prevent progression of the prolapse.
Pelvic Floor Muscle Exercises
Pelvic floor muscle training is critical to addressing symptoms such as urinary or fecal incontinence, or prolapse. This type of exercise includes strengthening the muscles that support the bladder, uterus and rectum as well as the muscles around the abdomen and hips. Often times strengthening these core and leg muscles can significantly improve pelvic floor muscle strength. The goal is to improve strength and endurance, increase circulation to the soft tissues of the pelvis, distribute intraabdominal pressure evenly, alleviate incontinence and improve sexual function.
Research supports pelvic floor muscle training as being effective in reducing overall pelvic floor symptoms in women with prolapse. The aim of conservative management of POP is to decrease the frequency or severity of symptoms caused by prolapse, prevent it from becoming worse, and avoid or delay the need for surgery.
Biofeedback and Electrical Stimulation
In some cases, pelvic floor physical therapists may use biofeedback (via manual techniques or use of a machine with sensors) to help patients learn to contract and relax their pelvic floor muscles properly. This provides real-time information to the individual on whether they are performing the exercise correctly.
Posture Training and Breathing Techniques
Managing intraabdominal pressure is key for reducing or eliminating symptoms of prolapse. Altered posture or breaching mechanics can cause increased downward pressure on the pelvic floor, thereby increasing symptoms of prolapse. Breathing into all sides of the rib cage can help improve distribution of the pressure in the abdomen and thus reduce symptoms.
Manual Therapy
Hands-on techniques might be used by physical therapists to reduce tension and improve mobility of the pelvic floor muscles. This may include gentle techniques to impact the muscles and the fascia, or connective tissue, that make up the pelvic floor. This can help reduce discomfort and other symptoms.
Patient Education
Physical Therapists provide education regarding activities that occur in your daily life to help reduce the risk of increasing symptoms.
Pessary Fittings
In addition to exercise and manual therapy, some pelvic floor physical therapists are trained and certified to fit pessaries, offering patients an effective, non-surgical option for prolapse support. Pessary fittings are now within the scope of physical therapy practice in many states, allowing qualified PTs to assess, size, and fit pessaries as part of a comprehensive prolapse management plan.
What is a pessary, and how can it help?
Some individuals may benefit from additional support beyond physical therapy intervention. Pessaries are soft, silicone medical devices that are designed to provide internal support to the pelvic organs. They can be especially helpful in women who want to try a more conservative approach rather than surgery, or who may not be surgical candidates. Pessaries can provide immediate relief of symptoms. They can be fitted by a healthcare provider such as a physical therapist or urogynecologist.
Pessaries function by being inserted into the vagina to support the organs. They come in various shapes and sizes and are broken down into two categories:
Support pessaries - pessaries that need something to support them in place (either pelvic floor muscles or bony support), such as a ring pessary
Space occupying pessaries - pessaries that fill the vaginal cavity to remain in place, such as a cube pessary which uses gentle suction to stay in place
Some benefits to using pessaries include:
Symptom Relief: Pessaries can provide immediate relief of symptoms of prolapse, including pelvic pressure, bulging, and incontinence.
Non-invasive: Provide a non-surgical option for people who aren’t candidates for surgery or want to avoid it
Customizable: Pessaries come in a variety of shapes and sizes, so they can be tailored to the individual's needs.
Reversible: They can be removed at any time, making them a flexible treatment option for women who may want to try other interventions in the future. Some types of pessaries can be self managed by the individual, while others require assistance from a healthcare provider to remove it.
For many women, a pessary can provide immediate relief from prolapse symptoms while pelvic floor physical therapy addresses the underlying muscular and tissue weakness. The use of a pessary allows women to manage their prolapse symptoms on a daily basis, while physical therapy strengthens the pelvic floor muscles, helping prevent further organ descent and improving long-term outcomes. There is research that supports that combining pessary use with pelvic floor physical therapy can be more effective at improving prolapse symptoms and qualify of life compared to either approach alone.
While pelvic organ prolapse can significantly impact a woman’s quality of life, physical therapy and pessaries offer holistic options to manage symptoms and improve pelvic health. If you are experiencing symptoms of pelvic organ prolapse, you deserve to feel better! Our physical therapists can evaluate you and create a tailored plan to get you on the right path to improving your quality of life and getting your confidence back.
Written by Dr. Nicole Morteo, PT
Nicole is trained in pessary fittings and currently accepting new patients at MomLife Health and Wellness in Braintree, MA.
Sources:
IUGA/ICS Joint Terminology Report for Female Pelvic Floor Dysfunction (Haylen et al 2010)
6th International Consultation on Incontinence
Limbutara W, Bunyavejchevin S, Chiengthong K. Patient-reported goal achievements after pelvic floor muscle training versus pessary in women with pelvic organ prolapse. A randomised control trial. J Obstet Gynaecol. 2023 Dec;43(1):2181061. doi:10.1080/01443615.2023.2181061
—